Why are Purpose and Engagement Essential to Enable Healthcare Outcomes Through IT?

Executive Summary
Executive role and organisation
Russell Hart, Senior Digital Applications Director for Queensland Health
- IT staff lacked visibility into the usability problems that frustrated clinicians and patients.
- Supporting patient outcomes required IT staff to understand the purpose of their role.
- Hybrid working deepened these issues because IT staff were now reluctant to visit sites
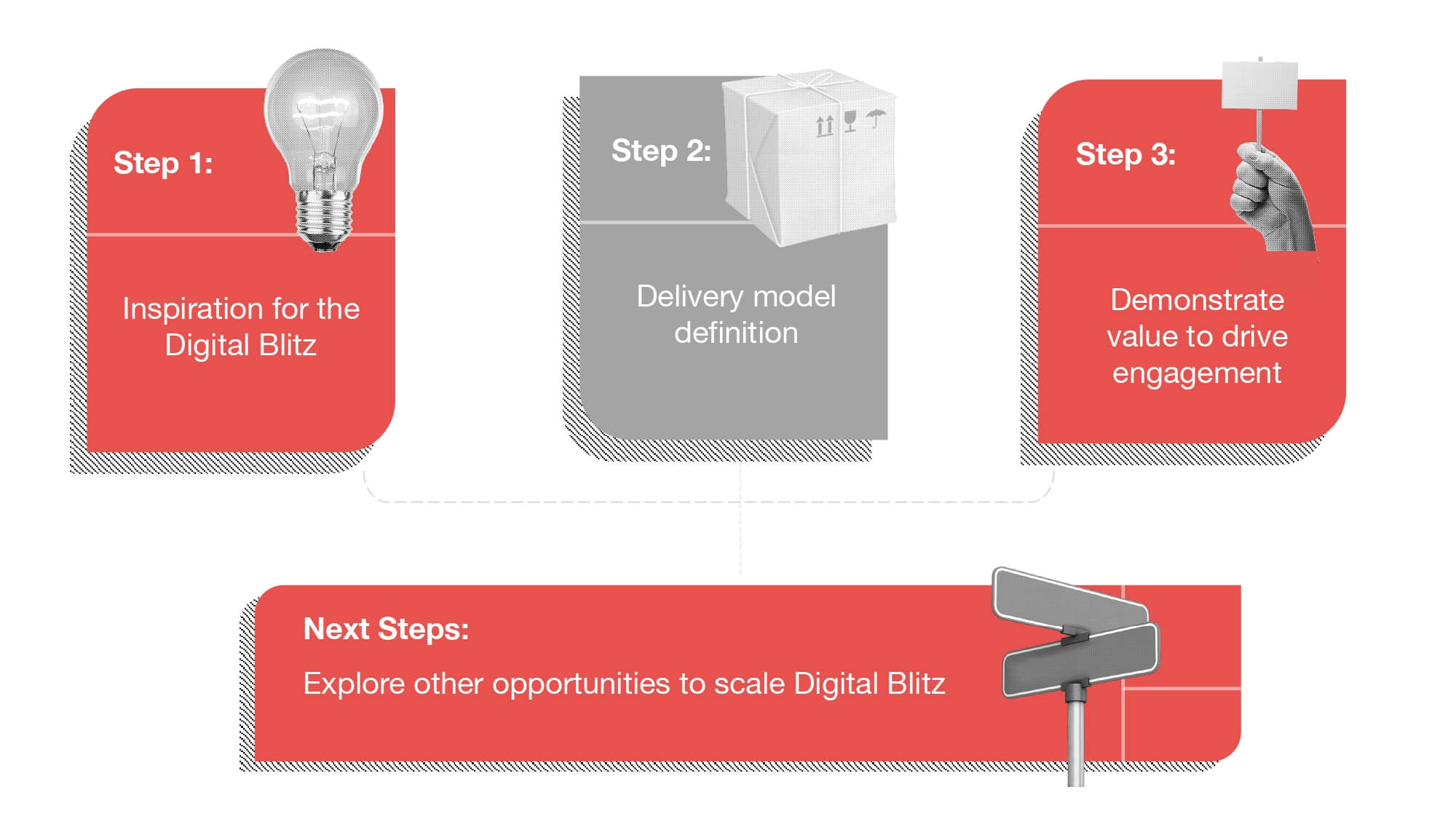
Delivering better healthcare outcomes required Queensland Health to review how IT engaged with the broader organisation. Changes in behaviour, ways of working, and focusing on purpose led to a program called ‘Digital Blitz’. According to Hart, taking small steps and demonstrating value during the journey can set up a stronger foundation for engagement and IT Outcomes. A chance encounter seeded the idea for Digital Blitz–an approach that involved:
- Creating small, multidisciplinary teams to determine the needs for Digital Blitz.
- Piloting Digital Blitz at smaller sites to build momentum and gain feedback.
- Demonstrating the value of Digital Blitz to drive engagement.
- Exploring other opportunities to scale Digital Blitz.
Digital Blitz [was a way] for staff to experience the reason why we are here: to support patient health. It’s about understanding how their work impacts clinicians and patients.” – Hart
- Initial onsite engagement took time to build: a simple fix helped drive momentum.
- The onset and aftermath of the pandemic required Hart to revisit the purpose of Digital Blitz.
- Adaptive change is leading to better engagement between IT and the frontline.
- Engagement builds understanding and empathy, which is delivering operating efficiencies and care outcomes.
- Better understanding is creating excitement and connection for IT teams.
- The outcomes delivered are driving executive engagements.
Background to the Initiative

Queensland Health
Queensland Health is the state’s largest healthcare provider, delivering integrated public health services for Queensland residents and visitors. These services are delivered through a network of 16 Hospital and Health Services and include hospital inpatient, outpatient and emergency services, community and mental health services, aged care services, and public health and health promotion programs.
The 2022–23 budget for Queensland Health exceeds $20 billion, which is devoted to maintaining and expanding the state’s healthcare infrastructure and services. The organisation has a workforce of more than 100,000 employees and serves the state’s 5.2 million residents. (Queensland Health, et. al 2022.) 1, 2, 3
Executive role
Russell Hart is the Senior Director for Digital Application Services at Queensland Health. His experience delivering healthcare technology solutions over the past two decades ensures he understands patients and staff needs.
The ‘Digital Blitz’ program aims to deliver better health outcomes for frontline staff and improve patient care based on his understanding of these needs. The purpose of this program is to overcome the engagement barriers that have emerged between these teams, and to demonstrate the outcomes that can result from driving adaptive change within the organisation.
How adaptive change can overcome resourcing challenges and priority conflict
Competing business priorities and IT talent shortages are the top challenges facing Chief Information Officers (CIOs) and Chief Digital Officers (CDOs) in healthcare and indeed across all sectors. These issues (depicted above) are described in an ADAPT Sector Analysis, published in August 2022.
Based on the responses of 290 Australian CIOs and CDOs, ADAPT finds that these challenges lead to problems with funding, enabling, and articulating the value of adaptive change. By embracing adaptive change, CIOs and CDOs can drive greater purpose and engagement, to deliver better outcomes for the people they serve.
According to Robert M. Wachter, MD and Chair of the National Advisory Group on Health Information Technology in England:
Many … mistakenly believe that implementing health IT [is] a simple matter of technical change … [where] in fact, implementing [it] is one of the most complex adaptive changes.”
Wachter references the work of Ronald A. Heifetz, MD. According to Heifetz, technical change is straightforward, in that it implements a clear set of instructions to solve an unambiguous problem. By contrast, adaptive change is needed to deal with complexities in requirements, engagement or accountability.
Adaptive change is messy but necessary. In healthcare, adaptive change will require shared ownership and understanding across IT, frontline and corporate functions. Adopting adaptive change can improve user experience by solving complex IT issues that often arise in healthcare. (Heifetz 20094 and Wachter 20165)
In this analysis, we will examine adaptive change as it relates to Queensland Health and how it informed the approach the organisation adopted.
We will explore the major catalysts, lessons learnt, and the business outcomes achieved, with a particular focus on how the organisation improved engagement between IT and frontline staff.
Catalysts

IT staff lacked visibility into the usability problems that frustrated clinicians and patients
The primary catalyst was to improve the usability of IT for key stakeholders. According to Hart, his key stakeholders are the organisation’s frontline clinical and administrative staff.
But until he pursued Digital Blitz, his team lacked visibility into technical glitches, which caused usability problems for frontline staff. Part of the problem involved system configurations and workflows that did not match how staff used the applications in practice. In addition, clinicians were too busy to call the helpdesk.
These disconnects were demonstrated in a consultation Hart shadowed, with permission:
The clinician … was explaining the care pathway to a patient, but the screen was signing out every minute. We found a fix…, which changed how clinicians provide consultations.”
Supporting patient outcomes required IT staff to understand the purpose of their role
The second catalyst involved understanding. Hart wanted his team to make connections between the activities they undertook and the purpose of those activities in delivering patient outcomes.
Understanding purpose required greater focus on the use of technology and less on the technical aspects of change. Hart recognised that to develop this understanding, his team had to be aware of the context in which these services were consumed.
Hart shared an example of the Smart Devices team visit to Longreach, where the very remote town’s nurse takes on multiple healthcare roles:
The team asked her if she uses … any smart devices. [The nurse] said we have three devices…; we did not know what to do with them or how to get them to work.”
This experience highlighted the need to deliver technology services that were easier to use, taking into account differing levels of digital literacy.
Hybrid working deepened these issues because IT staff were now reluctant to visit sites
The final catalyst emerged later. The onset of the COVID-19 pandemic required IT staff to work remotely and after almost three years of this delivery model, staff were now reluctant to revisit frontline centres. This reluctance compounds the original engagement issues that Digital Blitz was designed to address. Hart recognised that this required a new approach to scale Digital Blitz.
Hart said:
Hybrid [working] and COVID … reduced the opportunities for staff to experience the reasons we are delivering IT services: making a difference to patient health.”
Our discussion of Hart’s approach to adaptative, rather than technical change, considers these organisational catalysts. We will then explore the challenges and lessons learnt, concluding with the key outcomes.
Approach
A chance encounter seeded the idea for Digital Blitz
The idea for Digital Blitz was born out of a chance encounter Hart had at the roadside in 2019. When he called roadside assistance, he saw that the technician was accompanied by a corporate employee as a ‘ride along’.
Why was the corporate employee there? He wanted to know how customers consumed the organisation’s services and what support was needed by frontline staff engaged in service delivery. It was necessary to understand the challenges customers were facing and the frustrations frontline staff were experiencing. This provided insight into how these experiences (customer, colleague) could improve.
When I called [roadside assistance] … he [attended with] a ride along. It gave him ideas about what they [could do] in head office to help the people who deliver the services.” – Hart
Observing frontline staff’s activities would give Hart greater insight into how technology services might be improved. As a result, his staff would have a better sense of the purpose of their role and the clinical outcomes they would achieve. Next, we describe how Hart sought to replicate this idea in his organisation.
Create small, multidisciplinary IT teams to determine the needs for Digital Blitz
The next step was to create small, multidisciplinary teams to determine the needs for Digital Blitz. By developing multidisciplinary teams, Hart was able to create a delivery model that encompassed an understanding of the usage issues and potential solutions for technology services delivery to the organisation. The competencies of these teams included:
- application management and digital services design
- human capital management and payroll
- helpdesk, customer care and support.
During this pilot phase, Hart introduced Key Performance Indicators (KPIs) that incentivised his staff to visit sites and experience the real reason for delivering IT Services. Defining this delivery model allowed Hart to test Digital Blitz and learn if it would match demand from the frontline.
Pilot Digital Blitz at smaller sites to build momentum and gain feedback
Creating this delivery model provided Hart with the confidence to pilot Digital Blitz. Piloting the initiative at smaller sites in regional or remote locations helped to build momentum. The pilots gave Hart confidence that he was on the right path, helped him capture direct feedback from frontline staff, and helped define the scale of the opportunity.
Hart stated:
Before we went ‘Big Bang’ at Redcliffe, I was doing weekly product orientated visits to regional and remote locations to see how [our] systems were used.”
It was this confidence that allowed Hart to tackle a more structured approach, which we describe next.
Demonstrate the value of Digital Blitz to drive engagement
Digital Blitz creates engagement between IT and frontline staff to support patient outcomes. This is purpose in action; leading by example. The momentum gained in those early pilots gave Hart the license to tackle the solutions required at Redcliffe Hospital.
This purpose in action is demonstrated in a video about Digital Blitz. It shows Hart leading a team of 40 staff at Redcliffe Hospital to solve the most frustrating problems of frontline staff.
Hart states in the video:
Digital Blitz is all about getting our technologists face to face with clinicians and nurses to fix all of the niggly issues as we move through the hospital.”
At this point, the pandemic intervened and the challenges that arose from it will be discussed in the following section. First, we will explain the next steps Hart expects will help scale Digital Blitz.
Next steps: explore other opportunities to scale Digital Blitz
After relaunching Digital Blitz, Hart is considering its scalability. In addition to visiting medium-sized hospitals, provided he can drive momentum, he is looking at two other options to scale the program:
- delivering these engagements to other corporate functions
- exploring ecosystem opportunities across other parts of the Department of Health.
There is value beyond the organisation in these options. Scaling Digital Blitz across the Department’s functions will impact allied and ancillary services and help deliver better, more efficient technology services across the care ecosystem.
Hart stated:
I concentrate on the clinicians who are treating our patients. But there could be great benefit for doing the same for corporate or across the department. The question is: who would drive it?”
Challenges and Lessons Learnt

Initial onsite engagement took time to build: a simple fix helped to drive momentum
The challenge: In the early stages of Digital Blitz, Hart provided frontline staff with an app to schedule time with his team when they were onsite. The intent was to ensure the correct solutions and skillsets were onsite on the day of the visit, and to conduct a trend analysis of technology usage issues.
But when the team were onsite at Redcliffe Hospital, feedback from frontline staff suggested there were no technology issues to resolve. In part, this may have been due to nurses’ workload, as they were more focused on care outcomes and less on recalling the submissions made through the app.
The lesson learnt: Conversations help to unearth the main frustrations. By talking with frontline staff, Hart and his team were able to identify technology issues related to printing, patient care and payroll systems. Based on those requirements, Hart’s team was able to provide immediate solutions and build momentum for the remainder of the visit. According to Hart:
When we first got there …, the nurses said: ‘we don’t really have a problem.’ I thought ‘oh no, this is going to be a bust.’ Then someone shared a printing issue … and it snowballed from there.”
The onset and aftermath of the pandemic required Hart to revisit the purpose of Digital Blitz
The challenge: In early 2022, Hart recognised the engagement between IT and the frontline had diminished, due to the peculiarities of remote working. Also, waves of COVID were passing through Queensland, further reducing the opportunities for engagement.
The disconnect between IT and frontline staff arose because technical experts could not see the additional value provided by face-to-face engagement compared to working remotely. This resulted in staff missing opportunities to visit frontline centres.
Staff need to be where healthcare is being delivered to really make a difference. You can’t do that from home.” – Hart
The lesson learnt: These renewed engagement issues required Hart to revisit the purpose of Digital Blitz. This involved promoting the earlier, successful experience at Redcliffe Hospital and demonstrating why being onsite with frontline staff is important.
Staff that experienced these new opportunities were enthused, saying it was not something they wanted to miss.
I’ve had some little wins where I have organised visits out to retrieval services. Because that was exciting…, it has got the ball rolling, there was that buzz again,” Hart recalled.
Business Outcomes

Adaptive change is leading to better engagement between IT and the frontline
This adaptive approach to change leads to better engagement between IT and frontline teams. By engaging with clinicians and talking through their frustrations, IT can solve these problems rather than triaging via online forms. Larger hospitals also see the value of these engagements. Although these site visits will require more time and cost to deliver, the cost-to-value is proven. As Hart explains:
By putting … these programs in place …, [our IT teams] experience exactly what goes on in the wards. You can’t put a price on the relationships that we forged with clinicians.”
Engagement builds understanding and empathy, which is delivering operating efficiencies
Engagement builds understanding. By understanding the context of where and how services are being consumed, IT staff can design better services that deliver operating efficiencies. Two examples highlight these gains:
- Emergency department clinicians did not have the technology resources they needed in a space away from patients. There were consoles in each of the wards, but clinicians needed privacy to avoid causing alarm to the people receiving care.
- Cardiology nurses had to walk from the bedside to the nurses’ station whenever an alarm sounded, as the alarms were not visible around the ward.
Resolving the first issue was cost neutral; the second cost about $10,000. The first fix involved removing unused consoles from the bedside and supplying the right resources where they were required.
The second involved installing several large screen monitors that were visible from anywhere in the ward and would allow the nurse to go straight to where the care was needed. Both solutions saved clinical time, enabling better patient care. The first solution supported an increase in patient admissions and discharges.
It is not always about the money: the improvement [is in] … the patient flow. How do you put a price on that?” – Hart
Better understanding is creating excitement and connection for IT teams
Developing this understanding in IT is creating a better connection with frontline staff. As one of the frontline managers explains in the video shared earlier, Digital Blitz provides a venue to solve problems. This understanding helps IT teams to see purpose in action, leading to excitement and technology services that are more usable. This excitement comes from seeing how technologies are helping frontline staff to care for patients. As to usability, Hart shares an anecdote from the Smart Devices team:
The Smart Devices team realised that they had to change how they delivered their product. Now, everything is set up: A clinician can take the device out of the box and it works.”
The outcomes delivered are driving executive engagements
According to Hart, Digital Blitz was less about the costs of improving engagement and more about how his team can improve patient outcomes. He has the budget to support and scale the initiative, which includes everything from pre-planning to onsite visits. As Hart recalls, Digital Blitz is supported by senior executives in the organisation:
I have the budget that I need, but we’re not really talking about costs. We are talking about how we deliver this in the context of patient safety and the safety of my staff. The Deputy Director General is enthused and supportive.”
Executive Actions
Hart initiated Digital Blitz as the result of a chance encounter. His strategy involved improving IT teams’ understanding of clinicians’ frustrations and connecting their role to patient outcomes. Adaptive change underpinned these goals. As Hart developed his delivery model, piloted it at smaller sites and then gained momentum, his approach emphasised connecting clinicians and technologists to deliver patient care. Two challenges emerged:
- Engagement takes time but sometimes simple fixes can create momentum.
- The purpose of Digital Blitz had to be re-examined because of pandemic-driven hybrid working.
Digital Blitz delivers for clinicians in both experience and efficiency, for patients in terms of their care outcomes, and for IT staff in terms of understanding their essential role in these areas. The business and clinical outcomes are less about the costs and more about the care pathways. Further progress will follow within the context of ensuring patient safety and the safety of Hart’s staff.
Hart shares this final message for organisations seeking to pursue adaptive change:
Don’t underestimate spending time with your customer. As an example, our SQL team leader had a light bulb moment making a connection between what they do in the back end and how that helps clinicians.”
Footnotes:
- ‘Queensland Health: About’, Queensland Health, publication date unknown, accessed on September 22, 2022
- ‘2022-2023 Queensland Health Budget’, Queensland Government, 23 June 2022, accessed on September 22, 2022
- ’Snapshot of Queensland: High level summary data for Queensland in 2021’, Australian Bureau of Statistics, 28 June 2022, accessed on September 22, 2022
- R. Heifetz, et. al, ‘The Practice of Adaptive Leadership: Tools and Tactics for Changing Your Organization and the World‘, Harvard Business Press, 2009, accessed on 30 September 2022
- R. Wachter, ‘Making IT Work: Harnessing the Power of Health Information Technology to Improve Care in England‘, National Advisory Group on Health Information Technology in England, NHS England, 2016, pp5, 10, 14, 22, 36, 38, accessed on 16 September 2022









